One in eight.
One mommy waiting for preschool pickup.
One woman in your Target checkout line.
One mini-van maven in the Starbucks drive-thru queue on any given morning.
One of your best friends.
One in eight women today suffer from infertility.
At age 30, my pedestrian knowledge of the subject was limited to something I’d heard about a “friend of a friend.” At age 32, I became one in the eight; I was diagnosed with secondary infertility due to Diminished Ovarian Reserve (read: fewer eggs than a 32-year-old should have), in addition to male factor (read: hubby issues), too. Given our circumstances, In Vitro Fertilization (IVF) was our best option.

Being the control freak that my friends, family, doctors, and most of mankind constantly tell me I am, I needed to find out ALL OF THE INFORMATION on my diagnosis, treatment options, holistic approaches, pricing, odds of success, and everything in between…and ASAP.
So, I educated myself to expert-level status.
But more significantly, I became an advocate.
I strive to give strength to my #InfertilitySisters. To broaden the conversation. To break the stigma. And to help spread knowledge amongst the “seven in eight” (see what I did there?).
And trust me, living it firsthand, there is a stigma. Part of this, IMHO, is due to the simple lack of information and education about infertility and treatments. Though I’m an open book about my personal journey, the questions (and sadly, support) from friends and family are few and far between. People are uncomfortable around this incredibly common women’s issue.
Perhaps you are curious but confused. Unsure of what to say to a friend, but want to be there for someone you love. If so, read on.
From infertility to miscarriage and then some, I’ve been there. To honor the National Infertility Awareness Week I’ve devised what I’m calling “IVF 101;” a Q&A on common fertility questions (specifically surrounding IVF, my personal path).
“So what exactly is IVF?”
Cue Lil’ Jon shouting “SHOTS!” … Literally!
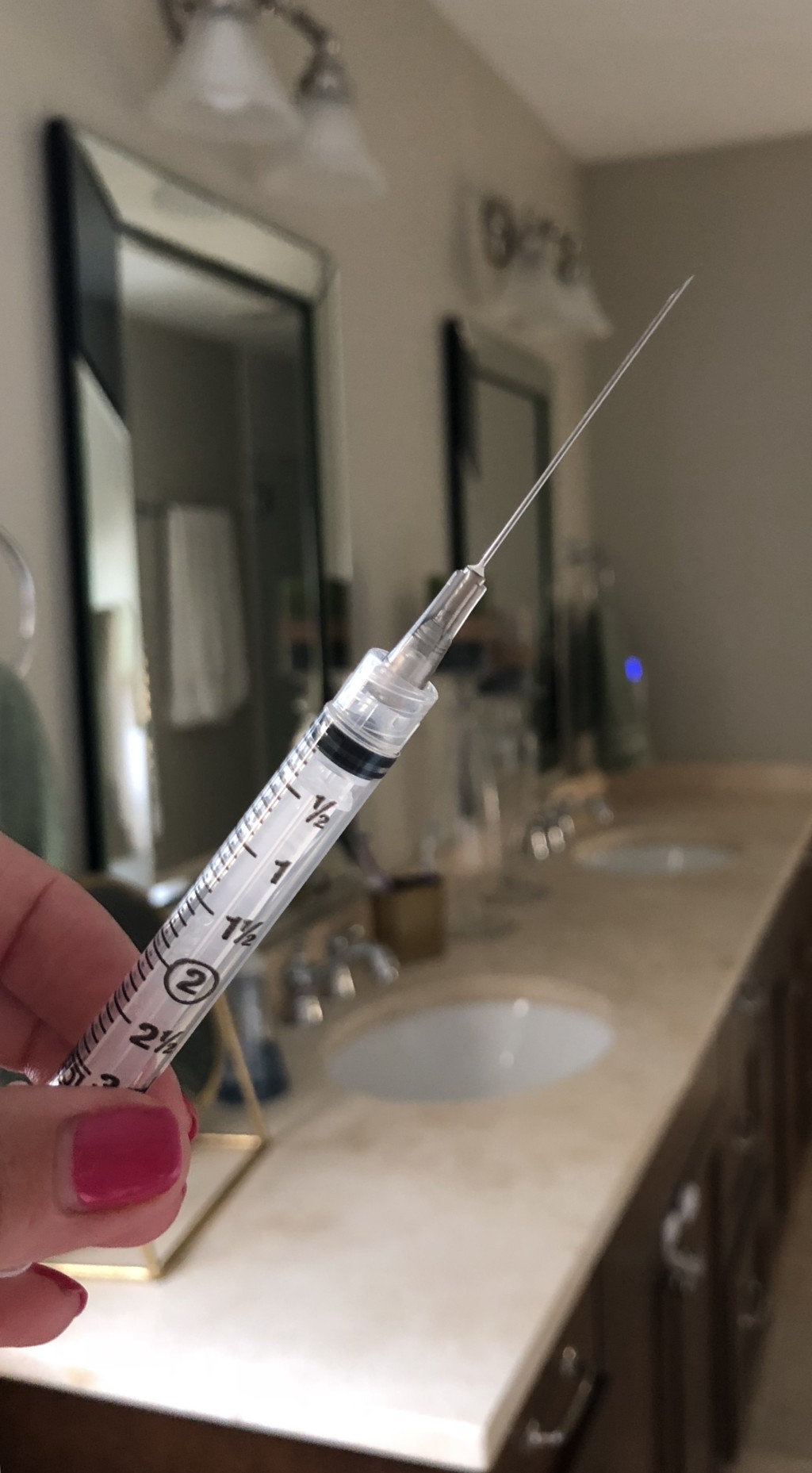
Arguably the most drastic and invasive of the medical intervention options for infertility, IVF first involves a “stim cycle” or “retrieval round.” Many friends have asked me about my “egg harvesting,” which, in a sense, I suppose this is. But the former are the proper designations for this aspect of treatment.
During these 10ish days of good times, I inject myself with anywhere from two to six shots of hormonal cocktails each day, straight to the gut. Getting used to the physical pain was easy; it’s the high-running emotions that make the struggle really real.
The goal: the hormones I inject stimulate my ovaries to grow an abnormal amount of follicles. Once my follicles are pumped and plumped, I’m given some sleep-sleep juice and go under for doc to remove my eggs – side note: each follicle should contain an egg – with a super long needle. Fun!
Next up, the lab experts, aka “embryologists” mix my eggs and hubby’s sperm in a process called fertilization. This is where the magic happens, and embryos are formed.
As soon as three to five days later, this embryo-soon-to-be-fetus can be transferred back into my uterus and begin growing! Most recently, I’ve chosen to “freeze all” embryos and do an FET (frozen embryo transfer) the following month; a way to let the body – and mind – take a break from the stress that is IVF.
“When will you know if you’re pregnant?”
About one to two weeks after my embryo transfer, I get a blood pregnancy test done to confirm if the embryo took. However, unlike a natural pregnancy, the testing doesn’t stop with two pink lines. I go in for several repeat tests, to make sure my HCG (a.k.a. pregnancy hormones) are increasing, and at the right pace. Early ultrasounds and other monitoring (and more drugs!) go on for at least ten weeks or so. The process is pretty grueling from a mental POV; it’s definitely challenging to get excited and enjoy your pregnancy when there are so many anxiety-triggering “check-ins.”
“Are you going to have twins/triplets/be the next Octomom?”
Probably not. Yes, multiple births are more common when using fertility drugs than conceiving naturally (for most women). But, single births are still the majority in both scenarios.
Most reputable doctors today will transfer two embryos max for the safety of mama and babe. With a single embryo transfer, my chance of pregnancy is about 20-25%. Pretty dismal, right? Transferring two slightly ups these odds, and also the chance of twins. Of course, all of this is highly dependent on age and a host of other factors.
“So, do you get to choose, boy or girl?”

In a nutshell, no again. Many people have heard that certain testing determines gender. While this is true, the actual reason embryos are tested is to weed out abnormalities caused by genetic conditions.
Though I’ve done this testing in the past, if I’m lucky enough to have a “choice” of embryos to transfer back, the no-brainer for me is to select the embryo with the highest grade, regardless of gender. Happy, healthy baby is my number one goal.
“But you’re so young, do you really need IVF?”
There’s a common anecdote that fertility “falls off a cliff” at age 35 — false.
For some, it’s 25, and others, it’s 45. 35 is just a misleading average we’ve all come to accept. I am a champion of early fertility testing for all young women for this exact reason.
And age is so unrelated in many infertility cases. Reproductive aging can happen prematurely (me: ‘waves hand’). Other issues include Polycystic Ovary Syndrome, Endometriosis, and Luteal Phase Defects. Some women have ovulatory conditions or recurrent pregnancy losses. About 30% of couples seeking intervention have male factor issues. And a staggering number of couple’s deal with the dreaded “unexplained infertility” diagnosis. The list goes on.
So, telling us to “relax” or “stop trying and it will happen,” you see, is actually not helpful but also so not true.
“But you had a child just fine two years ago, why do you need IVF now?”

Secondary infertility – having issues after the natural conception and live birth of at least one child previously – accounts for up to 30% of all infertility cases in the U.S. Shocking, I know. So while it’s not a dumb question, it can be insensitive. There are several reasons why a woman can no longer conceive or carry a baby to term after having a perfectly normal pregnancy and birth, and, unfortunately, it happens quite frequently.
“Isn’t this super expensive? How can you afford it?”
Yes and umm…still trying to figure out the second part. IVF treatments are costly. An average “cycle” comes with a price tag of around $25,000 when paying out of pocket. Since only about 15-20% of companies in the U.S. offer any sort of insurance assistance (and if they do, it’s pretty piddly most of the time), the majority of patients face enormous bills.
But, this doesn’t apply to all employers; local companies including Comcast, Quicken Loans and The University of Michigan are standouts in offering top fertility benefits. And to that, I say, “Bravo!”
From fundraisers to selling hand-crafted goods and hardcore budgeting, the families I know going through fertility treatments are the definition of resourceful. Still, the cost is the single largest barrier for people wishing to seek treatment.
One final disclaimer: I realize that all women struggling to grow their family are not as open as I am, and that is 100% ok. I am committed to sharing and breaking down barriers in this field but respect everyone’s right to privacy when it comes to their health and their bodies. You do you, girls!
I hope this overview helps you to avoid feeling silly asking a question and gives you more confidence in offering support to friends in need. More questions? Ask away in the comments below, slide into my DMs on Instagram, or check out Resolve.org, the utmost resource for infertility.
Ok…class dismissed!
This week is National Infertility Awareness Week and we at Detroit Mom want to make sure you feel supported. Continue reading some of our infertility content here. We welcome you to also join our Infertility and Loss Support Group on Facebook.
*Note: Kelsey originally wrote this post in 2018 and has since welcomed a rainbow baby who is turning two next month.











Love you! Thank you for this honest post.
love you shelbs!